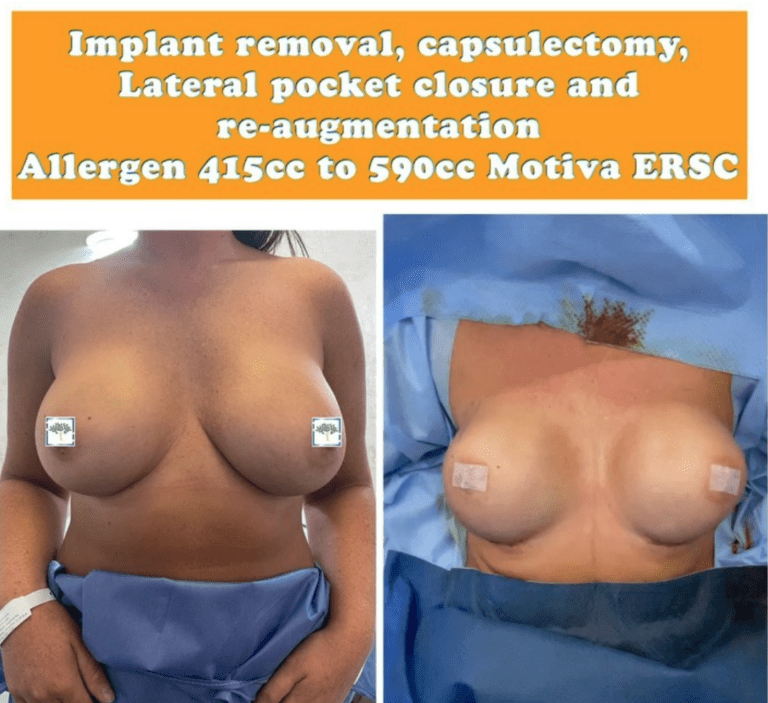
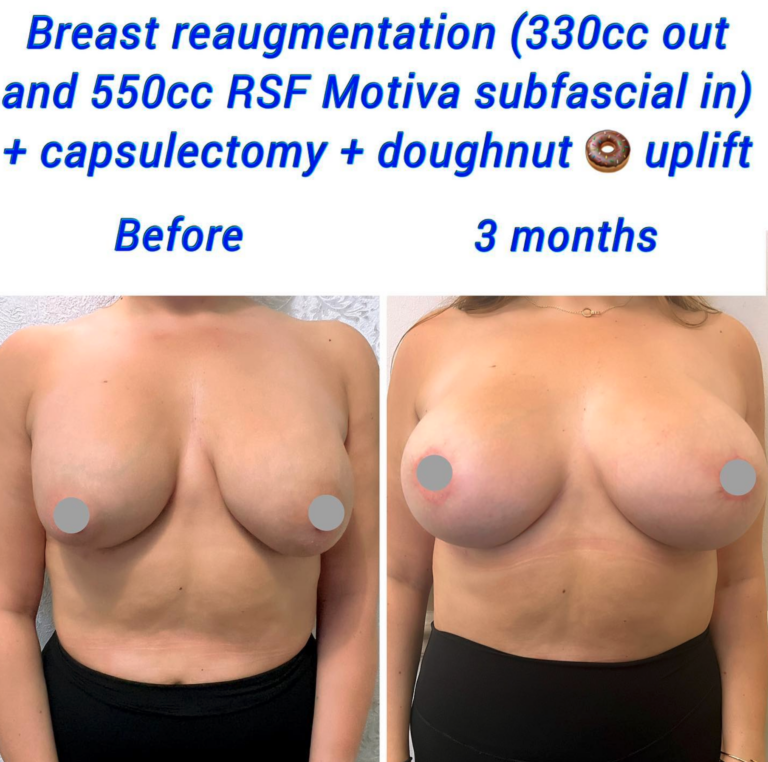
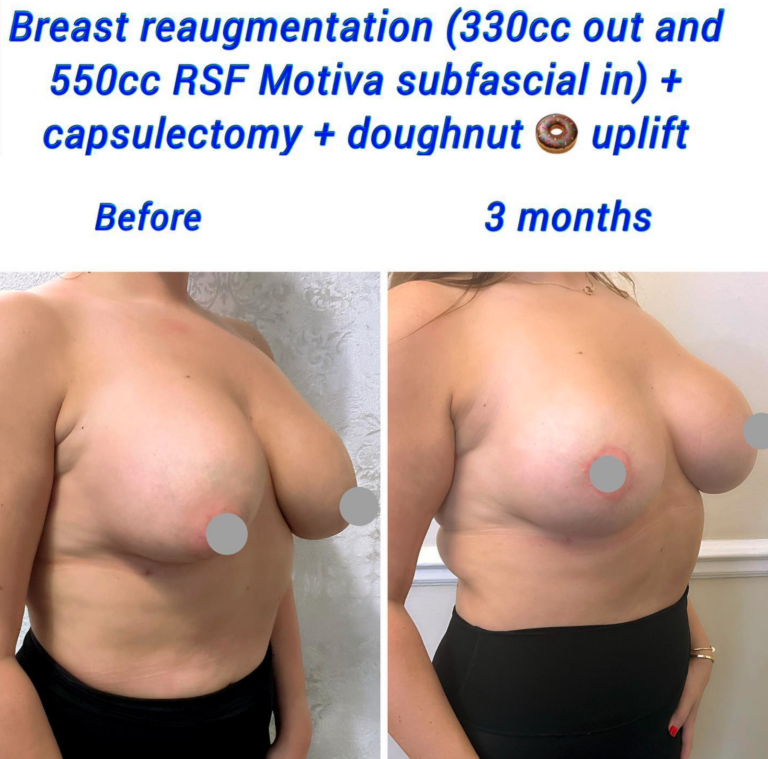
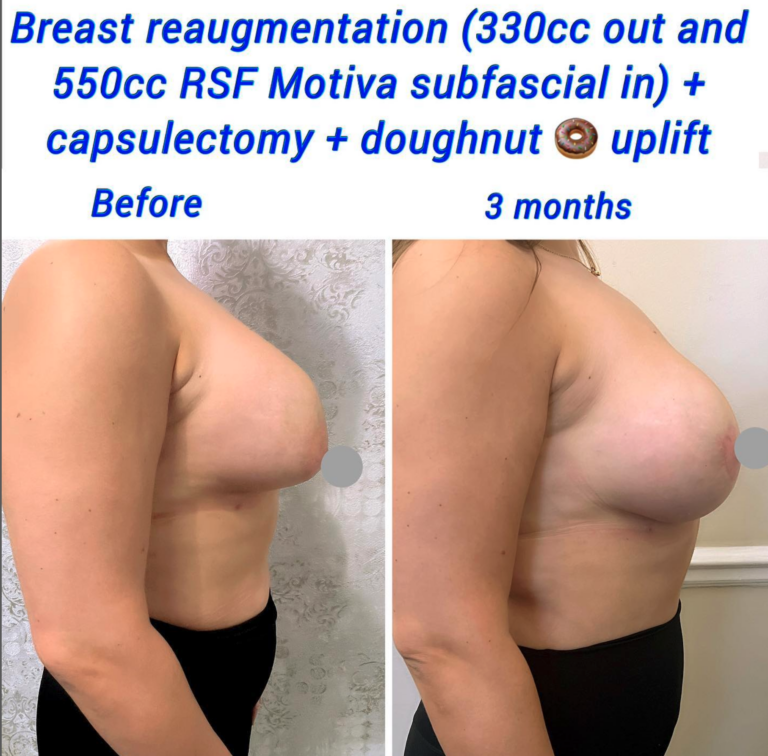
The body forms a protective capsule around any foreign object inside of it. The protective capsule is made of thick tissue. Following breast augmentation, the body treats breast implants as foreign objects, forming a capsule that helps keep them in place.
For many people, this capsule may feel soft or a little firm. However, for some, the capsule can tighten around the breast implants leading to a condition called capsular contracture, which may need surgical treatment known as capsulectomy.
Breast Capsulectomy: Quick Overview
- Surgery Time: 1 to 3 hours
- Anaesthetic: General
- Hospital Stay: Same-day
- Dressing and Garments: Dressings changed at 1 week and removed at 2 weeks, wear compression garment for 6 weeks
- Time Off Work: 1-2 weeks
- Exercise: 6 Weeks
- Mobile: 1 day
- Washing: At least 72 hours
- Sleeping Position: On back up to 2 weeks
- Full Recovery: 6 weeks
What is a Capsulectomy?
Capsulectomy is a surgical procedure to remove the hardened and thick tissue that forms around a breast implant, known as capsular contracture. Capsulectomy can be performed alongside breast implant removal or breast re-augmentation.
What is Capsular Contracture?
Capsular contracture is scar tissue that usually forms around a foreign object like a breast implant. Under normal circumstances, this scar tissue is thin, pliable, soft and sometimes can’t even be felt. Capsular contracture occurs when the scar tissue gets so thick that it tightens around the implant, squeezing it and making it feel firm.
Capsular contracture is a potential breast implant surgery complication. But is capsular contracture dangerous? While the condition isn’t fatal, it can change your breasts’ appearance and result in chronic pain. Capsular contracture can occur in anyone, regardless of how qualified your surgeon is.
The risk of capsular contracture increases the longer your breast implants remain in place. Saline and gummy bear implants are believed to have lower contracture rates than non-cohesive saline implants. At the same time, there is a lower risk of developing the condition if you have submuscular implants, and the same goes for textured implants. Severe cases of capsular contracture are managed through surgery.
What are the Causes of Capsular Contracture?
Women who undergo breast implant surgery will develop scar tissue around the implants to keep them in place. However, a few will develop capsular contracture. It is not clear why the condition develops only in some women. Still, there is an assumption that it could result from an inflammatory response that causes the body to produce excess collagen fibres.
Some people are more at risk of developing capsular contracture than others. For instance, people who’ve had radiation therapy are at an increased rate, but usually, the risk increases the longer you stay with breast implants. In addition, your genetic disposition might also increase your risk of developing it.
The risk of capsular contracture might also increase if the following occurs:
- Biofilm caused by bacteria forms
- Hematoma or blood build-up during surgery
- Seroma or fluid build-up under the skin
- Breast implant rupture
What are the Signs of Capsular Contracture?
Capsular contracture symptoms range from mild to severe. Mild cases present as mild breast firmness that usually goes unnoticed; some patients even love the firmness. Women who experience mild symptoms have breasts that are firm enough not to defy gravity or experience sagging and drooping over time.
Severe symptoms present as breast hardening accompanied by changes in the appearance of the breasts. The changes include an abnormal increase in breast projection, increased roundness with the outlines of the implants visibly noticeable through the skin and breast contour distortion. One may also experience sensation changes that range from hard and cold to painful. Such women will avoid physical touch like hugs because their breasts are too sore.
Usually, capsular contracture cases are identified through a grading system.
- Grade I – the breasts are soft and appear natural in shape and size.
- Grade II – the breasts feel a little firm but overall have a regular shape and size
- Grade III – breasts are firm, and the shape and size appear abnormal
- Grade IV – a severe stage where the breasts are hard, painful to the touch and size and shape are abnormal
Capsular Contracture Treatment Options
Capsular contracture treatment involves surgery if the symptoms are severe. Three surgeries may be performed, including breast implant capsulotomy, capsulorrhaphy and capsulectomy.
Capsulotomy
In comparison to capsulectomy, capsulotomy is a less invasive procedure if the capsular contracture is not severe. The procedure involves the removal of the breast implant plus a part of or all of the capsule. During breast re-augmentation, the implant is replaced after. However, you have the option to remove breast implants without replacement.
The procedure can either be open or closed. During open capsulotomy, you plastic surgeon makes an incision in the breast pocket and removes the breast implant and capsule. The procedure can range from 1 to 3 hours. Closed capsulotomy, on the other hand, though rarely performed, involves external compression to break up the capsule.
Capsulotomies are also done to open up the breast implant capsule pocket in certain dimensions. If you decide to have breast surgery for larger implants, capsulotomy is performed to increase the dimensions of the breast pocket to help accommodate the larger implants.
Capsulorrhaphy
Capsulorrhaphy involves adjusting the capsule or breast pocket dimensions, usually with sutures. For instance, where the breast pocket is stretched out, distended or too big, sutures help tighten the redundancy.
In case of implant malposition, sutures tighten that pocket section so the implant rests in an ideal location. The most common implant malposition is where the implant, over time, leads to lateral displacement, whereby the weight of the implant causes the tissue to thin out and stretch.
In such cases, larger implants are not the solution to restore fullness. Smaller implants or a breast lift at the same time can help tighten the skin reducing the risk of gravity causing the breasts to sag. Other implant malpositions that capsulorrhaphy can treat include symmastia (implants too close to each other) and breast fold malpositions.
Capsulectomy
Capsulectomy is a more invasive procedure than the two and involves the removal of all or part of the capsule. The surgeon can perform either partial or complete capsulectomy. During capsulectomy, the old implant is removed, plus the thickened scar tissues and a new implant is put in. While the procedure is effective, there is a risk of capsular contracture recurrence. To improve the outcomes and reduce recurrence risk, the surgeon may decide to:
- Use brand new implants
- Switch to submuscular pocket with mastopexy if the breast implants were sub glandular
Capsulectomy, while releasing the scar tissue, causes the thinning of the breast tissue envelope. So, in reality, the procedure may increase implant perceptibility and sagging over time.
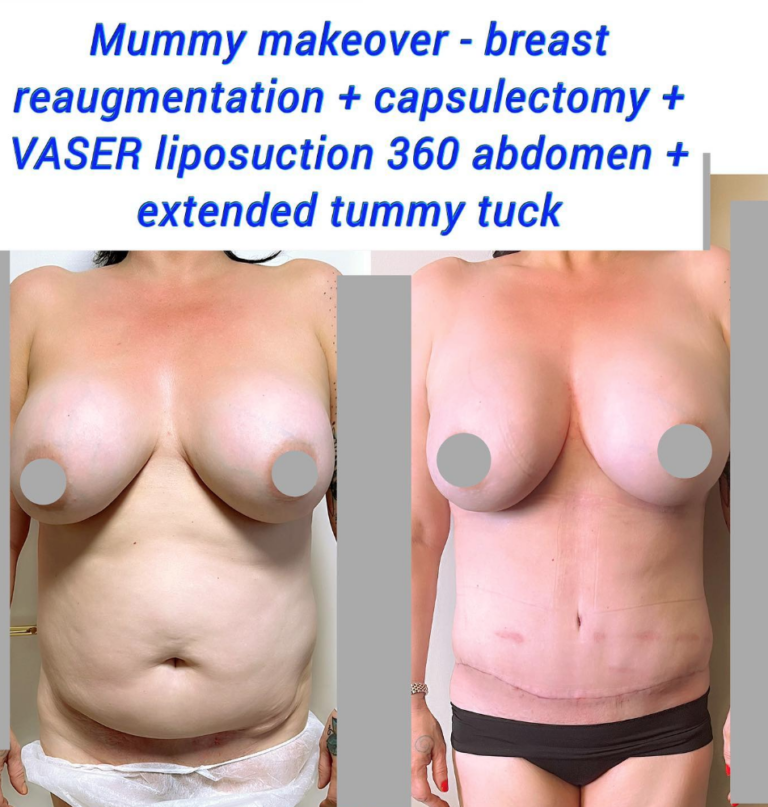
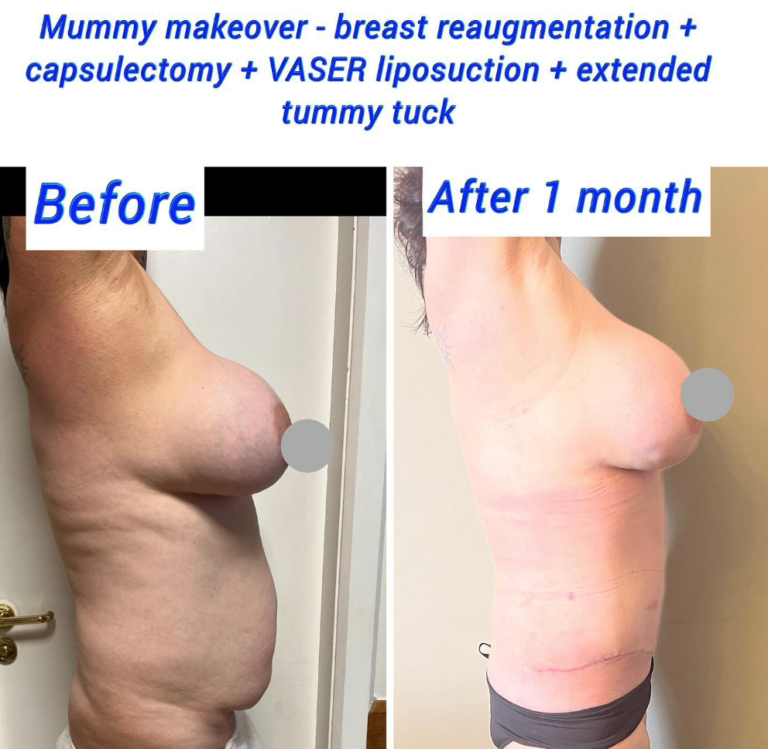
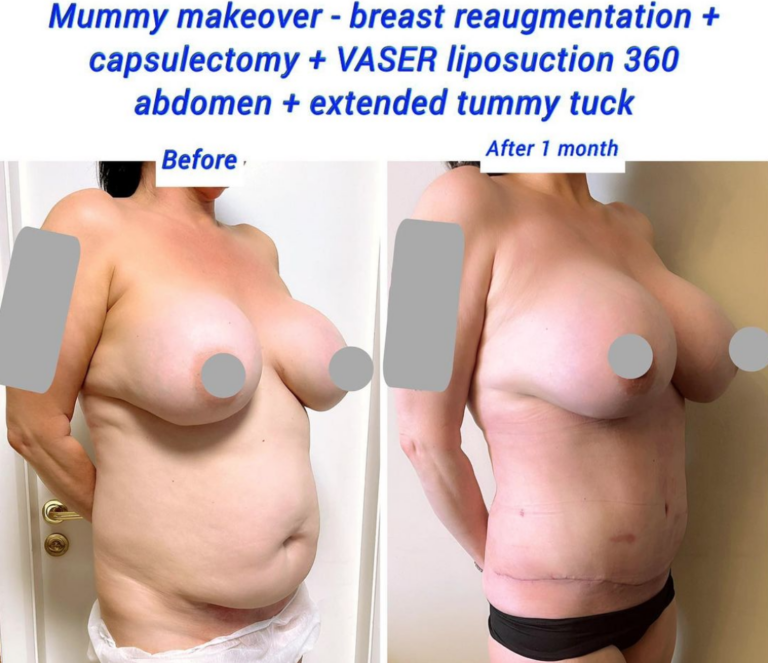
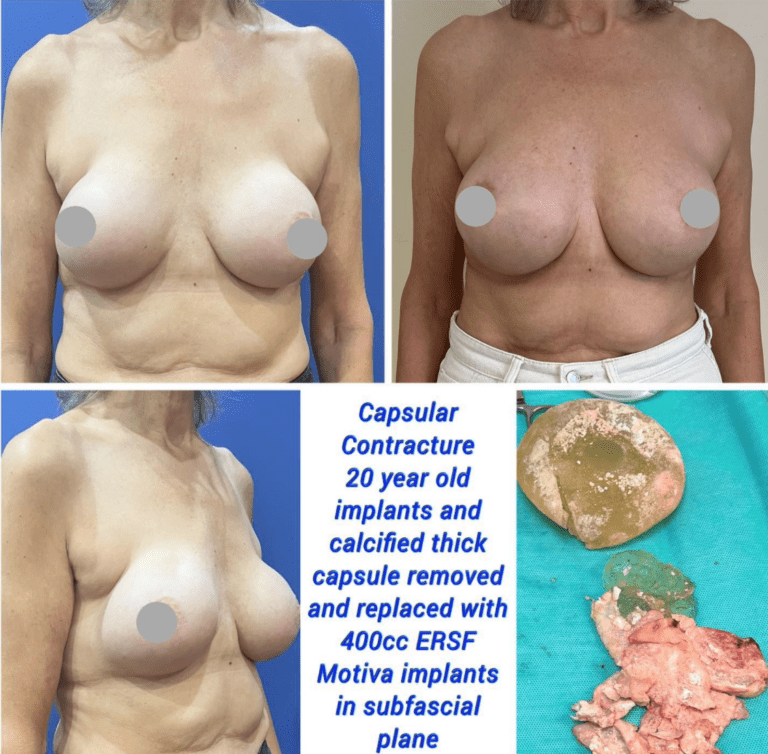
Before and After Capsulectomy
Capsulectomy, Capsulorrhaphy and Capsulectomy Risks and Complications
Potential capsulectomy risks and complications include:
- Infection
- Bleeding
- Hematoma
- Anaesthesia risks
- Skin and or fat/necrosis
- Fluid accumulation
- Pain
- Swelling
- Poor wound healing
- Poor scarring
- Nerve injury
- Contour irregularity
- Seroma
- Over/under correction
- Asymmetry
- Damage to other structures
- DVT
- PE
- Chest infection
- Need for further surgery
- Changes in nipple sensation
- Capsular contracture recurs
- Breast implants issues
Breast Surgery at Our Harley Street Breast Clinic
Talk to a Harley Street plastic surgeon today if you have breast implants and are worried about implant-related problems like capsular contracture.
Depending on your condition and the severity, different treatments are available to address it. When you reach an informed decision with the help of your plastic surgeon, you can be on your way to recovery.
A qualified plastic surgeon will assess your situation, give recommendations, and guide you on the best path to address the condition.
Reach out today to book a consultation and have all the knowledge you need to make the best decision that works for you.
Further Reading:
- Effects of Textured Breast Implants: What You Need to Know
- How to Choose Between Breast Augmentations, Lifts, and Reductions
- What is Breast Re-Augmentation?
- 7 Questions to Ask Before Your Breast Augmentation
- Can You Breastfeed After Breast Surgeries?
- How to Prepare for Breast Augmentation Surgery
- What You Need to Know About Breast Screening with Breast Implants
- How Can You Treat Capsular Contracture?